Crohn’s disease is one of the main types of inflammatory bowel diseases.
This condition is relapsing and remitting in nature which is related to the fact that there can be periods with no symptoms and then periods with symptoms presenting.
Crohn’s disease can impact any part of the digestive tract, from the mouth to the anus. However, the most common areas affected are the terminal ileum (the end of the small intestine) and the colon (the large intestine).
The inflammation in the gut is understood to be caused by a combination of factors. [Source: Pubmed]
Causes of Crohn’s Disease
While not fully understood, the development of Crohn’s disease appears to stem from a combination of factors.
These are:
- Genetic susceptibility
- Environmental factors
- Gut bacteria
The disturbance in the interaction between these factors results in a change in the immune response and damage to the lining of the digestive tract. [Source: Pubmed]
Genetics and Crohn’s Disease
On average 12% of those diagnosed with Crohn’s disease have a family history of the condition. [Source: Pubmed]
It’s also been noted that those of Ashkenazi Jewish heritage is 3-4 times more likely to develop Crohn’s disease than non-Jewish populations. [Source: Pubmed]
Those with the lowest risk are those of African-American and Asian heritage. [Source: Pubmed]
Gut bacteria and Crohn’s Disease
Changes in the gut microbiome have been noted in those with Crohn’s disease.
The general alteration in the balance of the gut microbiome is referred to as dysbiosis. There are key changes that have been reported. These are a reduction in Bacteroides and Firmicutes bacteria.
Alongside this, an increase in Gammaproteobacteria and Actinobacteria has also been reported. [Source: Pubmed]
Specific strains of E Coli have also been found in those with Crohn’s disease, appearing in 65% of chronic intestinal lesions. [Source: Pubmed]
These have the ability to cross the gut lining, impacting the cells that line the digestive tract as well as provoking the immune system. This provocation of the immune response may be central to the inflammatory response in inflammatory bowel disease. [Source: Pubmed]
This is also combined with a reduction in Faecalibacterium prausnitzii, a key beneficial bacteria with anti-inflammatory properties. [Source: Pubmed]
The understanding of the involvement of the gut bacteria in Crohn’s disease is supported but specific factors. This includes the fact that the location of the lesions in the gut wall are largely in the areas where the bacteria are most concentrated.
Additionally, with the use of antibiotic being favourable during moderate flares. [Source: Pubmed]
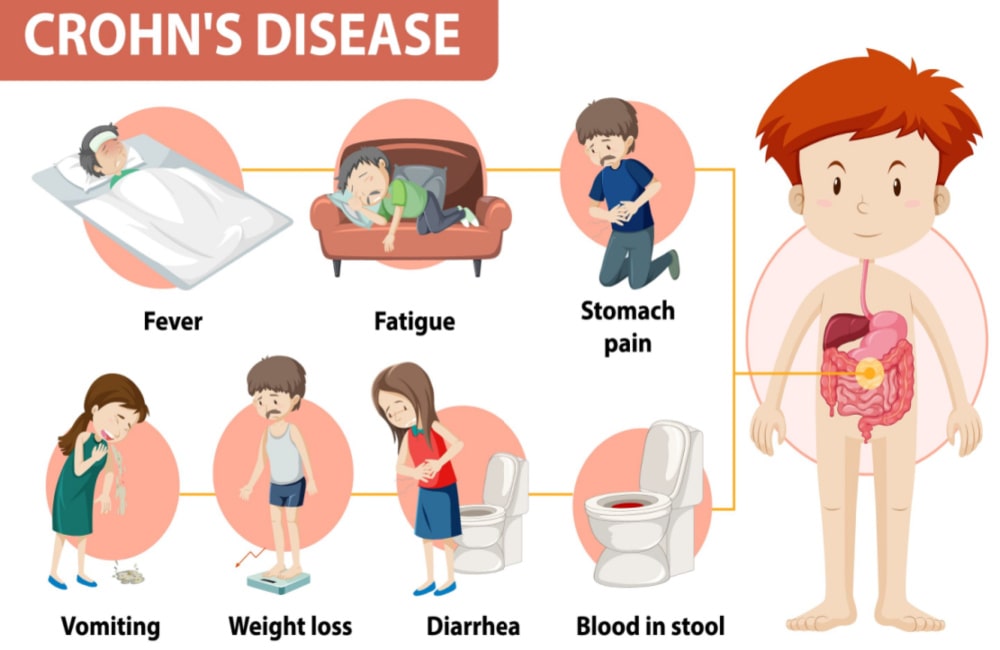
Symptoms of Crohn’s Disease?
The severity of symptoms depends on the location of the disease, the severity of the inflammation and disease behaviour.
The common symptoms of Crohn’s disease include:
- Diarrhoea
- Abdominal pain
- Weight loss
- Fatigue
- Malnourishment
In those with inflammation in the large intestine bleeding or bloody diarrhoea can also be present. [Source: Pubmed]
Additionally, in up to half of the cases of Crohn’s disease symptoms outside of the digestive tract may also present. These can be symptoms in the eyes or joints. [Source: Pubmed]
Complications of Crohn’s Disease
Population based studies have indicated several predictors of a worse outcome of the condition. While the reliability of these factors reliability has been questioned, they include:
- Ileal or ileocolonic location of the inflammation
- Extensive small bowel disease
- Rectal disease
- Perianal lesions
- Early structuring or penetrating disease
- Young age at diagnosis
- Smoking [Source: Pubmed]
The severity of the condition can lead to medication changes and the increased likelihood of requiring surgery. [Source: Pubmed]
Medications for Crohn’s Disease
The medications prescribed for Crohn’s disease vary depending on the severity of the condition as well as the response to previous medications.
The most commonly used pharmaceuticals in Crohn’s disease are:
- Corticosteroids
- Immunosuppressants (thiopurines [azathioprine and mercaptopurine] and methotrexate)
- Biologicals (anti-TNF [infliximab, adalimumab, and certolizumab pegol]
- Anti-adhesion molecules (vedolizumab) [Source: Pubmed]
Supplements for Crohn’s Disease
Specific natural supplements have been indicated to improve Crohn’s disease.
Sodium Butyrate
In a small study into the use of Sodium Butyrate, a compound with anti-inflammatory benefits, 53% of the group achieved remission over an 8-week period. [Source: Pubmed]
Curcumin
Curcumin is another anti-inflammatory supplement that can support those with Crohn’s disease. One study in those with mild-moderate disease activity has a 40% remission rate over an 8-week period. [Source: Pubmed]
Wormwood
The herb wormwood has been indicated via research to reduce the production of the pro-inflammatory chemicals that are produced in Crohn’s disease. [Source: Pubmed]
Conjugated Linoleic Acid
Conjugated linoleic acid (CLA) an omega-6 fatty acid was has been shown to reduce disease activity and increase the quality of life in Crohn’s disease patients. [Source: Clinical Nutrition]
Probiotics for Crohn’s Disease
While indicated to be beneficial in Ulcerative Colitis, the use of probiotics in Crohn’s disease are not as consistent. Some research even indicated that certain strains of probiotic bacteria may even increase the rate of relapse. [Source: Pubmed]
A study using the liquid probiotic Symprove indicated no benefit in Crohn’s disease, however, a benefit was found in those with Ulcerative Colitis. [Source: Pubmed]
An improvement in levels of inflammation was noted in one study using the probiotic blend, VSL3. This improvement was seen in those who started the probiotic early in the disease process. It’s also worth noting that in this study, the probiotic was taken for 365 days. [Source: Pubmed]