
The digestive system serves many roles. It’s responsible for the breakdown of food, the absorption of nutrients, and acting as a protective barrier.
The digestive tract is also home to a wide range of microorganisms. This collection of bacteria, yeasts, parasites (and others) is commonly referred to as the gut flora or the gut microbiome. [Source: Pubmed]
What is gut flora?
The gut microbiome begins to develop before birth, with colonisation occurring in the uterus.
The wide-ranging benefits of the gut microbiome include:
The number of genes that makes up the gut microbiome is several times higher than that of the human genome. Some research indicates that the microbial genome is 150 times higher than that of the human genome.
This leads to the gut microbiomes’ ability to carry out functions that the human genome has not, for example, nutrient extraction from food, and allows for the ability of humans to adapt to various environments. [Source: Pubmed]
When functioning optimally, this microbial ecosystem is in a balanced state, termed eubiosis. However, when imbalances develop, this is termed dysbiosis. This imbalanced state has been linked to several digestive conditions such as:
- Inflammatory bowel disease
- Celiac disease
- IBS
As well as other conditions such as:
- Obesity
- Metabolic disorders
- Type 2 diabetes
- Allergies
- Neurological disorders [Source: Pubmed]
Gut Flora Development
Soon after birth, the infant’s gut microbiome develops further. This is through the acquisition of microbes from foods, their environment, and contact with other humans. [Source: Pubmed]
This stage of development of the gut microbiome appears to be essential for the training of the immune system. It has been indicated that factors that negatively impact the development of the gut microbiome could increase the risk of several diseases later in life.
2 of the main factors that appear to impact the development of the infants gut microbiome are:
- The mode of delivery with a natural birth offers more benefits than a c-section.
- The infant’s source of nutrition with breastfeeding provides more benefits than formula. [Source: Pubmed]
A key factor relating to both of the above is the health of the mother’s gut microbiome, as the composition of the mother’s ecosystem strongly influences the infants. [Source: Pubmed, Pubmed]
Once this ecosystem is established, it remains stable throughout the majority of adult life, with changes becoming apparent in the elderly. [Source: Pubmed]
Also Read: How To Reduce Inflammation In The Gut
What damages the gut?
In adulthood, the gut microbiome can still be impacted by factors potentially leading to a dysbiotic state.
These include:
- Food/food quality
- Food additives
- Antibiotic intake
- Drug use
- Alcohol abuse
- Gastrointestinal disorders
- Infection [Source: Pubmed, Pubmed]
From a food perspective, the western diet is detrimental to the balance of the gut microbiome and can lead to a gradual shift over time.
This diet is characterised by:
- High levels of heavily processed foods
- Rich in fat, sugar, protein
- Rich in additives
- Low in nutrition
- Low in dietary (gut-friendly) fibre [Source: Pubmed]
This type of diet has been associated with an increased risk of Crohn’s disease, ulcerative colitis, and colorectal cancer. [Source: Pubmed, Pubmed]
This type of diet also leads to several changes that include a reduction of beneficial bacteria such as bifidobacteria and a reduction in the beneficial by-products of fermentation known as short-chain fatty acids. [Source: Pubmed]
Gut Imbalances
When stable, the gut microbiome support human health. However, when imbalances occur, this mutually beneficial relationship is lost. This imbalance is referred to as dysbiosis.
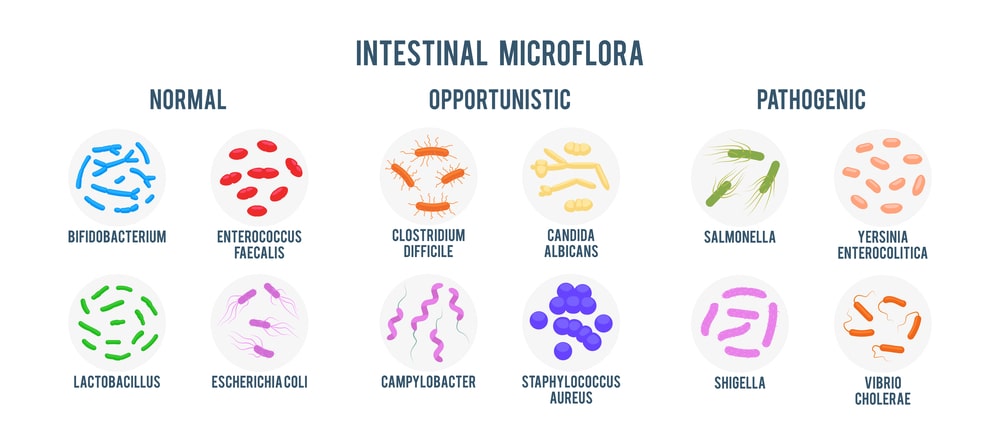
When this occurs, we can see reduced levels of the beneficial organisms and elevated levels of the potentially pathogenic organisms. Along with this shift in the balance, a reduction in the diversity of the ecosystem also occurs. [Source: Pubmed, Pubmed]
Dysbiosis is a general term; however, it can be divided into different forms.
Deficiency dysbiosis. This is a reduction of the beneficial species, which can be the result of long-term dietary patterns or antibiotics. This is associated with food intolerances. [Source: Pubmed]
Putrefactive dysbiosis. This involves an increase of putrefactive bacteria, which is often the result of a western-style diet. This can lead to the creation of products that may impact the gut and systemic health.
Fermentative dysbiosis. This often impacts those with IBS, those who have received antibiotics, and individuals who have a low level of fermentable fibres (such as FODMAPs) in their diet. [Source: Pubmed]
Susceptibility dysbiosis. This is associated with alteration in the gut that may lead to an altered immune response, altered motility, and inflammation, which has been linked to the development of inflammatory bowel diseases.[Source: Pubmed, Pubmed]
Fungal dysbiosis. This is characterised by the overgrowth of fungal species such as candida which is commonly promoted but the western diet. [Source: Tandfonline]
While there are several ways the gut microbiome may become imbalanced, restoring balance is essential to support overall gut health as well as systemic health. [Source: Pubmed]
Rebalancing the Gut Microbiome
Several strategies are involved in supporting and rebalancing the gut microbiome.
One key part of this approach is to address any of the modifiable factors already described that can lead to an imbalanced gut microbiome. For example, this includes a diet with the appropriate amount of fermentable fibre and not drinking alcohol to excess.
There are 3 factors that can be considered easily accessible therapeutic strategies for modifying the gut microbiome.
These are:
- Food/diet
- Probiotics
- Prebiotics [Source: Pubmed]
The conversation into the dietary approach to modifying the gut microbiome can be started with the Mediterranean diet. This is characterised by a diet rich in plant foods (vegetables, fruits, whole grains, herbs, spices). This also involves beneficial levels of non-digestible carbohydrates (fibres) that are fermented but the gut microbiome.
This leads to the production of beneficial compounds called short-chain fatty acids, which are responsible for approximately 80% of the energy requirements for the cells that line the gut.
[Source: Pubmed]Additionally, key nutrients such as zinc, folate, and vitamins D and A are seen as key to a healthy microbiome. [Source: Pubmed]
This template of diet may be at odds with a low FODMAP diet. This diet is often suggested for this with symptoms of IBS due to its ability to reduce the level of fermentation taking place in the gut.
Due to alterations in the gut in those with IBS, high levels of fermentation may not be tolerated and may lead to symptoms such as bloating. While this may reduce symptoms, a long-term low FODMAP diet can impact the gut microbiome negatively. [Source: Pubmed]
Probiotics
Probiotics are defined as “live microorganisms that, when administered in adequate amounts, confer a health benefit on the host.” Probiotics have been indicated to support a balanced gut when exposed to insults that may have otherwise resulted in dysbiosis.
These insults include prolonged antibiotic therapies and stress (both physical and mental).
The action of probiotics is far-reaching and includes:
- Supporting the immune response along the gut lining
- Inhibition of pathogens
- pH alterations
- Down regulating the immune response to food antigens
- Reduction in intestinal inflammation [Source: Pubmed]
There is also a difference between types of probiotics which allows for specific strains to be used in specific situations.
For example, the benefits of the friendly strain of E. Coli (Nissle 1917) include:
- Improving the intestinal barrier
- Reducing intestinal cell invasion by pathogens
- Supporting intestinal balance [Source: Pubmed, Pubmed, Pubmed]
Additionally, the fact that the probiotic yeast, Saccharomyces boulardii, is resistant to antibiotics makes it a good candidate for use alongside antibiotic therapy to limit alterations within the gut. [Source: Pubmed]
Prebiotics are considered non-digestible substances that, when taken in adequate amounts, produce beneficial effects by stimulating the growth of specific gut bacteria. [Source: Pubmed]
While these do not introduce bacteria to the gut, they support the gut environment leading to alterations that make the ecosystem less favourable to potentially pathogenic microorganisms. For example, they lead to a reduction in colonic pH, which results in an unfavourable environment for putrefactive bacteria.
Conclusion
Due to the range of imbalances that can occur in the gut microbiome, understanding the type of dysbiosis can lead to more specific administration of therapies. [Source: Pubmed, Pubmed]
While some factors, such as mode of delivery, are not-modifiable later in life, we do have clear interventions to address gut imbalances and rebalance the gut microbiome.
Working with a Registered Nutritional therapist can take the guesswork out of rebalancing the gut.






