If you’ve been diagnosed with IBS or SIBO, or have gut issues such as bloating or diarrhoea, you may have come across a low FODMAP diet.
This is a dietary approach to calm gut symptoms and to identify specific trigger foods for gut issues.
While this isn’t a long-term diet to follow in it’s strictest from, a short term intervention with a low FODMAP diet can dramatically improve quality of life. This is especially true when carried out under the care of a nutritionist.
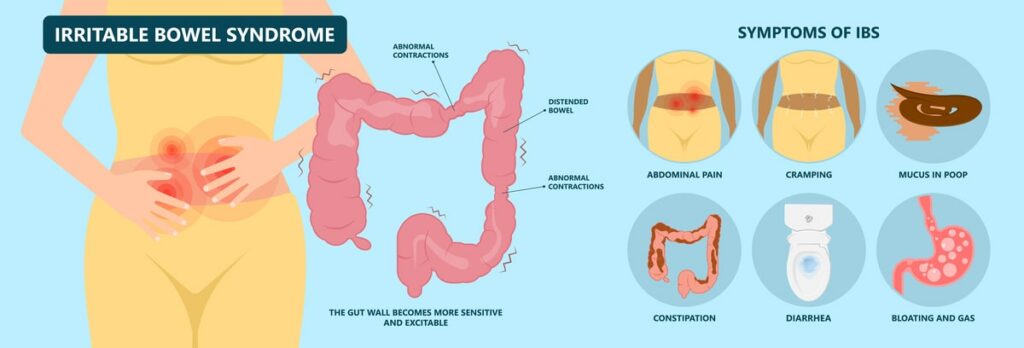
What are low FODMAP foods?
In those with gut issues, certain carbohydrates (fibres or sugars) may cause an issue and increase symptoms. These higher FODMAP carbohydrates are present in a wide range of healthy and natural foods. However, if the gut is irritated these foods may then lead to symptoms.
Therefore, a low FODMAP diet is a way to reduce high FODMAP carbohydrates and to take a wide range of trigger foods out of the diet to calm symptoms.
These are foods that contain fibres and sugars such as:
- Lactose
- Fructose
- Fructans
- Sorbitol
- Galactans
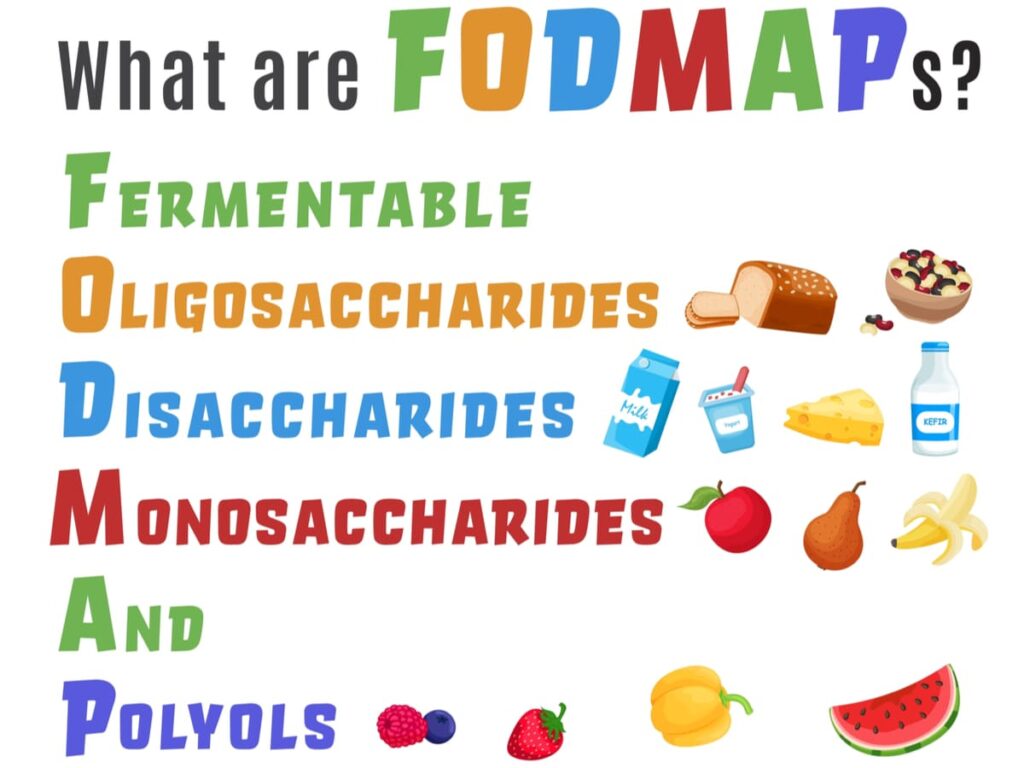
The types of carbohydrates are also references in the anacronym FODMAP which stands for:
Fermentable | Process through which gut bacteria ferment undigested carbohydrate to produce gases. |
Oligosaccharides | Fructans & GOS - found in foods such as wheat, rye, onions, garlic and legumes/pulses. |
Disaccharides | Lactose - found in dairy products like milk, soft cheeses and yogurts. |
Monosaccharides | Fructose - found in honey, apples, high fructose corn syrups, etc. |
And | |
Polyols | Sorbitol and Mannitol - Found in some fruit and vegetables and used as artificial sweeteners. |
What are the benefits of low FODMAP foods?
Underlying factors in the gut can lead to food intolerances. For the most part, those with IBS may have an intolerance to one (or several) high-FODMAP foods.
These underlying irritations in the gut can include:
- SIBO
- Dysbiosis
- Malabsorption
- Low-grade inflammation
- Visceral hypersensitivity
The factors mean that the high FODMAP carbohydrates are either poorly absorbed in the small intestine or poorly fermented due to imbalances in the gut bacteria.
An aspect of the diet that often sounds contradictory, is that the aim for long-term gut health is to eat a high-FODMAP diet. This is due to many of these high FODMAP fibres actually being beneficial to the gut microbiome.
However, in the short term, reducing these fibres can calm symptoms and provide more predictability for IBS symptoms while the underlying issue is addressed.
Even when following a low FODMAP diet, there should still be a focus on keeping the diet as diverse and as natural as is possible. These are 2 factors that help to support the gut microbiome and the health of the gut lining.
List of low fodmap foods
While there are restrictions when following a low FODMAP diet, there is a very wide variety of foods that can be included. These form a central part of the diet
- Fruits
- Vegetables
- Proteins
- Grains
- Dairy alternatives
- Beverages
These foods will each fall into the various categories of FODMAP
Low fodmap fruits
- Bananas, blueberries, cantaloupe, grapefruit, honeydew, kiwi, lemon, lime, oranges, and strawberries.
Low fodmap vegetables
- Bamboo shoots, bean sprouts, bok choy, carrots, chives, cucumbers, eggplant, ginger, lettuce, olives, parsnips, potatoes, spring onions, and turnip
Low fodmap proteins
- Beef, pork, chicken, fish, eggs, and tofu.
Low fodmap grains
- Oats, oat bran, rice bran, gluten-free pasta, quinoa, white rice, and corn flour.
Low fodmap dairy and dairy alternatives
- Almond milk, lactose-free milk, rice milk, coconut milk, lactose-free yoghurt, and hard cheeses.
Low fodmap beverages
- Low FODMAP teras include green, rooibos, peppermint, liquorice and black tea. Black coffee is also permitted on a low FOMDPA diet (however, coffee may be a trigger for other reasons in those with IBS).
High fibre low fodmap foods
A possible side effect of a low FODMAP diet is a reduction if fibres that support bowel movements. In some patients, this can lead to reducing motility and constipation appearing or worsening.
When starting a low FODMAP diet, ensuring fibre intake is maintained at around 30g per day is often helpful to continue to support motility as well as the microbiome.
Low FODMAP foods that are high in fibre include:
- Oats (16g of fibre in 1 cup)
- Kiwi (2g of fibre)
- Quinoa (5g in 1 cup cooked quinoa)
- Green beans (3.4g of fibre in 100g)
- Carrots (3g of fibre in 100g)
- Chia seeds (8g in 2 tablespoons)
These foods will be the lowest in FODMAP while still helping the gut and bowel movements. Often when constipation increasing we can start seeing changes in the gut microbiome so keeping an eye on fibre levels is helpful for the gut and microbiome.
Tips for shopping for low fodmap foods
Generally for most patients a week or 2 following a low FODMAP diet indicates how helpful this approach may or may not be. With this in mind, it’s not always crucial to understand every aspect of the diet before starting it.
One of the simplest ways to shop while following the diet is to have a list of 5 breakfast and 5 lunch/dinner meals. These can be rotated over the first phase of the diet.
The other approach that can be taken is to use the food list as a ‘pick-and-mix’ chart. By using the list in this way, a meal can be created by selecting a food or combination of foods from each section of low FOMDAP foods to create a meal.
This would look like selection 1 source of low FODMAP protein, 1 low FODMAP vegetable and 1 low FODMAP grain. This way a meal can be easily constructed without the need for recipes and harder-to-find ingredients.
Conclusion
While the low FODMAP diet may look complex, there are 2 things to remember.
The first is that it is a short-term diet, not a diet to follow for life. For most of my patients, a 1-2 week trial of the diet if often enough to understand how helpful this approach may or may not be.
The second is that working with a practitioner can make this process much easier. Not only to navigate the dietary side but also to get to the underlying cause of the symptoms.
Contact us today for a free assessment.
History
Updated by Martin Cohen, 2nd Nov, 2024
References
- Bellini M, Tonarelli S, Nagy AG, Pancetti A, Costa F, Ricchiuti A, de Bortoli N, Mosca M, Marchi S, Rossi A. Low FODMAP Diet: Evidence, Doubts, and Hopes. Nutrients. 2020 Jan 4;12(1):148. doi: 10.3390/nu12010148. PMID: 31947991; PMCID: PMC7019579.
- Syed K, Iswara K. Low-FODMAP Diet. 2023 Sep 4. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan–. PMID: 32965895.
- van Lanen AS, de Bree A, Greyling A. Efficacy of a low-FODMAP diet in adult irritable bowel syndrome: a systematic review and meta-analysis. Eur J Nutr. 2021 Sep;60(6):3505-3522. doi: 10.1007/s00394-020-02473-0. Epub 2021 Feb 14. Erratum in: Eur J Nutr. 2021 Sep;60(6):3523. doi: 10.1007/s00394-021-02620-1. PMID: 33585949; PMCID: PMC8354978.