What is IBS?
IBS stands for irritable bowel syndrome.
This is a common digestive disorder that has a range of symptoms related to digestive function.
How is the digestive system affected by IBS?
Rather than seeing IBS as something that does affect the digestive system, the question I like to ask about IBS is “What change in the digestive system is leading to the symptoms of IBS?”
What organs does irritable bowel syndrome affect?
We can divide the organs that IBS affects into 2 categories. Inside the digestive system and outside the digestive system.
Inside the digestive system, IBS symptoms can be present in:
- The oesophagus
- The stomach
- The small intestine and the large intestine
It is also being seen in research into the gut microbiome (the beneficial bacteria) that there is connection between IBS, the bacterial imbalances in the digestive system and how these can impact other organs throughout the body.
These organs include:
- The brain (anxiety, depression)
- The liver (NAFLD)
- The thyroid (hashimoto’s)

Does IBS cause poor digestion?
One of the common symptoms of IBS is poor digestion. There can be different ways to describe poor digestive.
These include:
- Bloating
- Diarrhoea
- Constipation
- Undigested food in the stool
These symptoms can be triggered from food but also emotional factors such as stress.

What causes IBS?
IBS symptoms can vary from person to person. However, when symptoms are present an underlying issue or imbalance can be considered.
These underlying issues commonly fall into 3 distinct categories.
Lifestyle & Environmental Factors
- Stress
- Circadian disruption
- Physical inactivity
Functional Imbalances
- Exocrine pancreatic insufficiency
- Low-grade inflammation
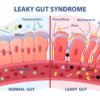
- Intestinal permeability
- Bile acid diarrhoea
- Chronic constipation
- Dysbiosis
- SIBO (Small intestinal bacteria overgrowth)
- Parasitic Infection
Nutritional Factors
- Carbohydrate intolerance
- Lactose intolerance
- Food hypersensitivity
- Non-celiac gluten sensitivity
- Nickel-related intestinal mucositis
- Vitamin D deficiency (5)
Irritable bowel syndrome foods to avoid
A dietary template that has been well researched for those with IBS is the low FODMAP diet.
FODMAPs are groups of carbohydrates (sugars and fibres) that are commonly poorly absorbed in the small intestine. These carbohydrates then travel to the large intestine where they are fermented by the beneficial bacteria and used as their energy source.
This fermentation is a healthy process and one that does not result in symptoms if our gut bacteria are in balance.
We commonly see that if there is an imbalance in these bacteria, excess gas is produced and symptoms of IBS follow.
These symptoms include gas, abdominal distention, bloating, nausea, diarrhoea and/or constipation, which can range from mild to debilitating.
FODMAPs Defined
| F | Fermentable. Poorly digested carbohydrates, such as FODMAPs, are broken down and fermented by bacteria in the gut and produce gases. |
| O | Oligosaccharides. This term includes fructans and galacto-oligosaccharides (GOS) found in wheat, onions, garlic, beans, and cashews. |
| D | Disaccharides. The double sugar, lactose, found in dairy products such as milk, ice cream, custard, puddings, and certain cheeses. |
| M | Monosaccharides. The “simple sugar,” fructose, when present in greater amounts than glucose in foods such as apples, mangoes, pears, asparagus, agave, and honey can lead to IBS symptoms. |
| A | And |
| P | Polyols. Naturally occurring sugar alcohols such as mannitol and sorbitol found in fruits, and vegetables, and also commercially produced sugar alcohols found in packaged foods:Sorbitol: apples, blackberries, peaches, and coconut waterMannitol: cauliflower and large servings of sweet potato and celeryXylitol, maltitol, sorbitol, mannitol and isomalt: sugar-free gum & candies, processed foods, and some dietary supplements and medications. |
Limiting these highly fermentable foods can be helpful as a short-term strategy to help manage symptoms.
However, the ultimate aim is to address the underlying issue so that the body can tolerate these foods. (6)
Who is at risk for IBS?
The most common 3 risk factors for developing IBS are if you:
- Are young. Most people first get IBS before they are 45 years old.
- Are female. Females get IBS almost twice as often as males.
- Have had recent food poisoning or gastroenteritis (7)
What are the symptoms of IBS?
Often those with IBS symptoms can experience a low level of symptoms most days.
However, an IBS attack or flare-up can occur which leads to an increase in the severity of symptoms.
These include:
- Bloating
- Pain/cramping
- Increased urgency
- Reacting to more foods
- Anxiety (8)
How is IBS diagnosed?
Once other conditions, such as inflammatory bowel disease, have been excluded IBS may be diagnosed based on certain criteria.
The Rome IV Criteria for IBS is as follows:
“Recurrent abdominal pain lasting, on average, at least 1 day per week in the last 3 months, associated with two or more of the following criteria:
- Related to defecation
- Associated with a change in the frequency of stool
- Associate with a change in the form (appearance) of stool” (9)
While these symptoms may indicate what the bowel is doing, it’s not offering any insight into why it’s doing it.
This is why many conventional options for IBS treatment can be very generic and not offer a deeper insight into the causes of the symptoms. (10)
What does your poop look like with IBS?
Having IBS does not mean that the appearance of poop will change it is fairly common for it to do so.
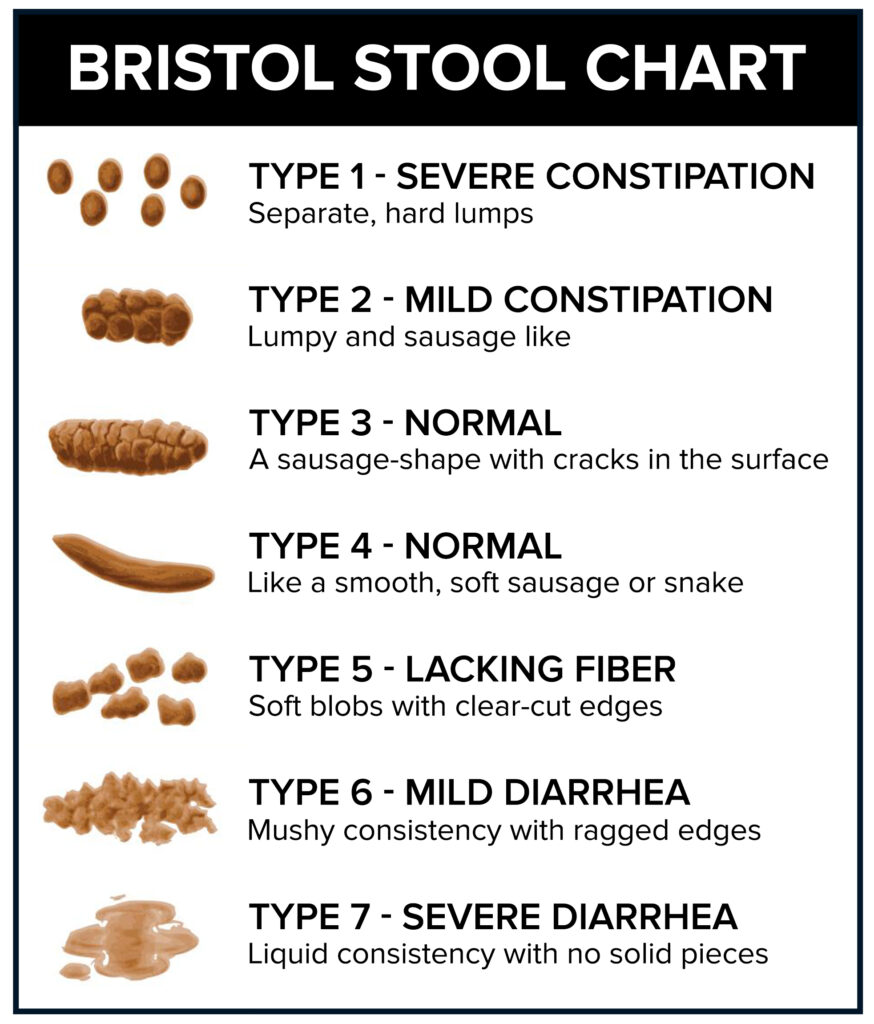
The Bristol stool chart was designed to help identify the appearance of the stool. For those with constipation their appearance of the stool can be towards the top of the chart, eg type 1.
With those with looser bowel movements being towards type 7.
It can also be common to see mucus in the stool as well as undigested food. (11)
IBS Treatments
There are various strategies to help calm IBS symptoms. These largely depend on the underlying issue and what is leading to the symptoms.
How is IBS treated?/ Irritable bowel syndrome treatment
The main components to supporting the foundations of digestive health and IBS are:
- Keeping the diet diverse in plant foods. The diversity of the diet supports the diversity of the gut bacteria, a key indicator of gut health.
- Limiting processed foods. Refined and processed foods impact the microbial balance and also the gastrointestinal environment.
- Limiting any aggravating foods. A low FODMAP diet may be helpful in the short term to help manage symptoms.
- Probiotics. Depending on the specific set of symptoms and underlying factors, various types of probiotics may help improve the health of the digestive system. (12)
How to cure IBS permanently
To permanently resolve symptoms of IBS, it’s important to address the underlying issue.
How to cure IBS in one day
IBS can be a complex condition and is unlikely to be cured in 24 hours. However, for some, limiting FODMAP can bring symptoms under control very quickly.
This often means someone can feel a great deal more comfortable whilst the underlying issue is addressed.
What are possible complications of IBS?
While IBS does not increase someone risk of developing colon cancer or inflammatory bowel conditions, there other potential complications.
IBS is associated with an increased risk of:
- Haemorrhoids. These may be causes by chronic constipation.
- Poor quality of life. Digestive symptoms can lead to disruption on a daily basis as well as unpredictable reactions to food.
- Mood disorders. In addition to the disruption to life and the frustration with symptoms, issues such as anxiety and depression may be the result of imbalance in the gut. (13)
Living with IBS
Living with IBS has many challenges, particularly when it comes to understand what foods cause the issues and living a stress-free life.
Irritable bowel syndrome diet
For some more specific information on diet and IBS you might like to read our article on Dietary guidelines for IBS.
References:
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4051916/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4056127/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5733421/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4051916/
- https://www.mdpi.com/2624-5647/1/3/27
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7468924/
- https://www.cghjournal.org/article/S1542-3565(12)00308-4/fulltext
- https://pubmed.ncbi.nlm.nih.gov/28541989/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5704116/
- https://www.nhs.uk/conditions/irritable-bowel-syndrome-ibs/diet-lifestyle-and-medicines
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3855407/
- https://pubmed.ncbi.nlm.nih.gov/31480656/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4051916/