IBS impacts a significant number of people around the globe impacting approximately 11.2% of the population with women being more affected than men. (Source: Pubmed)
The common symptoms include:
- Bloating
- Abdominal pain
- Changes in bowel patterns (constipation or diarrhoea) (Source: Pubmed)
While these symptoms can be very common, with many IBS sufferers the underlying cause can vary from person to person. This means that even though the IBS symptoms can be the same, the root cause and therefore the treatment strategy can differ.
Many people with IBS note that there are certain triggers that can worsen their symptoms with stress being one of them. For some, during stress periods their IBS symptoms can worsen yet for others stress can gradually impact IBS symptoms over a period of time.
A strong correlation also exists between the severity of symptoms and emotional factors such as depression, stress and anxiety. This indicates that if someone has a pre-existing presence of either low mood or anxiety their gut issues may be more severe. (Source: Pubmed)
This has led some researchers to indicate that IBS is a combination of an irritable bowel and an irritable brain. (Source: Pubmed)
The Development of IBS
The exact reason for developing IBS can vary but research has indicated several factors that can increase someone’s risk of developing digestive issues.
These factors include:
- Psychological stress
- Food reactions (intolerance or allergy)
- Intestinal infection
- Injury (e.g., abdominal or pelvic surgery)
- Intestinal immune disruption and/or inflammation
- Changes in the intestinal microbiota or bacterial overgrowth
- Abuse and early life learning (Source: Pubmed)
The alterations seen in the stress response can for some be a driving factor behind their symptoms. The communication between the gut and the brain is called the gut-brain axis and over-reactivity or under-reactivity along this communication pathway may lead to altered functioning of the gut. (Source: Pubmed)
What is Stress?
Stress is a term that was defined by Hans Selye in 1939. This term was used to describe responses within the body to threats. These threats can be physical (eg being chased by a predator) or psychological (eg: an argument with a loved one).
Short-term stress can activate the ‘fight or flight’ response. Here, when under threat the body prepares itself to fight off this threat (as it would if we were being chances by lion).
When this short-term stress passes the body activates a response to switch off the ‘fight or flight’ response and return to balance or homeostasis.
The issue we can now face in the 21st Century is that the stresses we experience stops being short-term and are more chronic in nature. This long-term stress places considerable strain on the body which makes it more challenging to return to balance.
Commonly in the modern age these stresses can social and emotional in nature. (Source: Pubmed)
Can stress cause diarrhoea?
While stress can make us feel more emotionally reactive and sensitive this can have an impact on how we eat. For some, this change in food habits can lead to unhealthier choices which may then directly impact gut health and possibly lead to gastrointestinal problems and altered bowel movements.
However, direct links between what is happening in the brain and how this then impacts gut health have been identified.
Research has indicated that stress has an impact on:
- Intestinal sensitivity
- Altered motility (the movement of the gut)
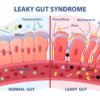
- Intestinal permeability (leaky gut)
- Mucosal immune activation
- Alterations in the central nervous system
- Gut bacteria imbalances (Source: Pubmed)
Stress and IBS (irritable bowel syndrome)
The role of gut bacteria is key for many aspects of health, including digestion and gut health. While many of these aspects are digestive in nature they also include areas outside of the gut such as helping the immune system as well as anti-systemic inflammatory processes. (Sources: Pubmed)
Specifically, within the digestive system alterations in these bacteria can lead to many of the central system symptoms in IBS. These alterations include changes to key groups of beneficial bacteria and a reduction in microbial diversity. These gut alterations might cause someone to feel more stressed.
This can also include increased sensitivity of the gut lining (leading to pain) as well as altered bowel motility (leading to constipation or diarrhoea). (Source: Pubmed).
One of the reasons for these changes has been indicated to be an alteration in the mucosal barrier. This is also called the gut lining. (Source: Pubmed)
One study in animals showed that when under high amounts of stress changes to the gut took place. These changes included:
- An increase in inflammation along the gut lining.
- Increase intestinal permeability
- Increase sensitivity and pain in the digestive system
As the gut microbiome also supports the stress response and the gut-brain axis this can also create a vicious cycle. This is where stress alters the balance of the gut bacteria but then the imbalanced gut bacteria alter the stress response.
This imbalance or impairment of the stress response may then lead to chronically elevated levels of cortisol which is highly associated with digestive symptoms. (Source: Pubmed)
Imbalances along the gut lining can also contribute to increased reactions to food. (Source: Pubmed)
How to treat stress-induced diarrhoea
Stress has also been shown to lead to an increase in the inflammatory process in those with inflammatory bowel diseases such as Crohn’s disease and Ulcerative Colitis.
While these conditions are distinct and different from IBS this research demonstrated how an increase in the stress response directly works to impact gut health. (Source: Pubmed)
How To Manage Stress
While often easier said than done stress management can often be central to addressing gut issues.
Areas and information that often needs to be reviewed include:
Setting Boundaries
In the 21st century with increased work and family pressures, we can be left with little time for ourselves. There can be a constant demand for our energy and our emotional resources which can often be hard to say no to. Setting clear boundaries and creating time and space for yourself can lead to making changes an easier process.
Stress Management
Practices such as meditation and yoga are often very helpful for calming the nervous system and have been shown to be as effective as a low FODMAP diet for managing stress and IBS symptoms (Source: Pubmed)
Diet
While in the short term, a low FODMAP diet may be helpful for someone to reduce the severity of their symptoms. A diverse high-fodmap diet can be key to supporting bacterial diversity and supporting the nervous system. This diet is best approached under the care of a healthcare provider such as a nutritional therapist. (Source: Pubmed)
Part of the approach with this diet is to encourage healthy eating practices while temporarily reducing certain types of fibre to manage symptoms.
Supplements
Specific strains of probiotics and prebiotics have not only been shown to support digestive health but may also support the stress response via the gut-brain axis. Using the right supplements can be a key way to treat the underlying cause of gastrointestinal problems such as diarrhoea. These underlying causes of IBS and diarrhoea include food intolerances as well as imbalances in the gut bacteria can (Source: Pubmed).
Gut Directed Hypnotherapy
When alterations in the gut-brain axis and the stress response have taken place, further support has been indicated to help reduce stress and improve IBS symptoms. Gut-directed hypnotherapy can be introduced through a qualified healthcare provider.
While stress can be a cause of IBS and diarrhoea, it can also start to cause alterations in the gut. This means that while stress can be the cause, the imbalances it contributes may also need to be addressed with appropriate diet, eating practices and supplements such as probiotics. (Source: Pubmed)
How long does stress diarrhoea last?
Diarrhoea that is caused by stress is usually described as acute. This means that it’s shorted lived and, in most cases, the gut symptoms calm down soon after the stress has passed without the need for treatment. For many, this may be before an important social engagement or when work stress increases. [Source: Pubmed]
If symptoms are persisting and continuing for days or weeks this can be described as chronic diarrhoea which may require a visit to a healthcare provider such as a doctor. This can be an important part of ruling out more serious causes of gastrointestinal symptoms. [Source: Medline]
Can you have diarrhoea with stress?
Many people with gut health issues such as IBS find that diarrhoea is often triggered by stress and anxiety. Not only does stress impact eating patterns which alone can cause a flare-up in IBS symptoms, but stress can also directly impact the gut.
The way that stress triggers the gut is partly via the gut-brain connection which is the main communication pathway between the brain and the gut.
When stressed, the body enters the ‘fight or flight’ response which involves the release of stress hormones. Not only can these enter the gut, leading to alterations in the gut bacteria but they can also influence bowel motility. These 2 aspects can be responsible for diarrhoea and IBS symptoms that increase with stress. [Source: Pubmed]
Conclusion
While there are clear links between stress and diarrhoea it’s important to take into consideration all other risk factors to help improve and resolve gut-related issues.
Diet, history of infection, sleep patterns and hormonal balance are all factors that can regularly be in need of further investigation to ensure a holistic approach to gut health.