Introduction: Understanding the Link Between Stress and Bloating
Stress, anxiety, and bloating. This seems to be a combination that often comes hand in hand. Very commonly, when someone is experiencing digestive symptoms of bloating, but also other symptoms of IBS (irritable bowel syndrome) such as cramping or constipation, these more emotional symptoms are present.
Can stress cause bloating or is it that the digestive symptoms are causing the stress? Often, it can be both.
The definition of bloating may also be worth clarifying. Strictly speaking, bloating is the sensation of pressure within the stomach, whereas the visible inflation of the abdomen is referred to as distention. While they can appear in isolation it’s more common for bloating and distention to happen at the same time [1].
Can stress and anxiety cause stomach problems?
Stress and anxiety are so common in our lives in the 21st century that we might not always be aware of them. Daily challenges, endless emails, and traffic jams, all contribute. The issue with these stressors becoming normal is that we stop noticing them. Our brains tune them out, however, they may still lead to health issues [2].
It’s also possible for ongoing and highly stressful experiences to contribute to stomach problems. These include the death of family member or the end of a relationship.
A very common theme for those with digestive symptoms is that they feel the stress in their gut. This can often happen before the stress is felt emotionally. The daily stresses can impact our digestive function via various biological pathways in the body.
This is the connection between the gut and the brain, but also the brain and the gut. This means that information is sent in both directions. Stress can not only alter bowel function but it can also lead to changes in the gut microbiome and changes in mood.
Stressful events and experiences can switch the brain into survival mode. This may then lead to a change in digestive function. Stress may also lead to increased pain perception, a factor that is closely linked to bloating. [3]
Cortisol and Gut Health
When under stress or feelings of anxiety begin to rise, our limbic system (the region of the brain with responsibility for memory and emotional responses) becomes activated. Once activated, this then signals to the adrenals glands to release the hormone cortisol.
Cortisol has many roles. These include altering metabolism to increase the energy available to escape the perceived threat. As well as increasing heart rate and respiratory rate, (to provide higher levels of oxygen to power the escape.) This is what we would consider the “fight or flight response”.
The fight or flight response is triggered by feeling under threat. When feeling threatened we are left with 2 options. To either fight the threat or to run away from it. In primal terms, this is the lion in the jungle that’s chasing us, but in modern terms, this is the 100 emails in your inbox.
In the gut, the cortisol can:
- Lead to microbiome imbalances, a key cause of bloating
- Alter transit time, possibly leading to diarrhoea and further microbiome imbalances
- Contribute to intestinal permeability (leaky gut)
- Impact nutrient availability [4]
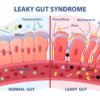
Stress and Leaky Gut
High levels of stress and the cortisol that are products can also impact our gut lining leading to increased intestinal permeability, also known as leaky gut. Here, the junction that connects the cells that line the gut lose its integrity, leading to:
- Gut compounds entering the bloodstream
- Changes to the gut microbiome
- Immune activation
As well as digestive symptoms, increased intestinal permeability has been linked to:
- Metabolic syndromes
- Liver disease
- Colitis
- Depression [5]
Most notably, an inflammatory component of the bacterial cell walls (called LPS) may pass through the gut and into the bloodstream. Once in the bloodstream, it may then contribute directly to anxiety, stress and depression.
This may create a vicious cycle where stress contributes to changes in the gut but then these gut changes increase stress.
Stress and Diet
Stress and sugar consumption are also linked which can then contribute to bloating as well as changes in the gut microbiome. Specifically, the consumption of high amounts of refined carbohydrates can alter the microbial balances in the digestive system. This has also been linked to a reduction in resilience to stress, meaning we are less able to deal with stress.
This can be exacerbated as commonly during periods of high stress or anxiety, foods higher in refined and processed carbohydrates are often consumed. The consumption of sugar improves feelings of anxiety in the short term, however, in the long term, it can lead to microbial disruptions.
This can be due to a diet that is higher in refined carbohydrates often being lower in the important fibres needed for the gut. This can result in an alteration to the pH of the bowel, creating an environment that allows less beneficial gut bacteria to thrive. [6]
Stress and the Gut Microbiome
Stress can alter the balance of bacteria in our digestive system. Even once this stress has been resolved the imbalance may still remain leading to digestive symptoms.
One of the main roles of the bacteria is to help us digest food, however, when the balances of the bacteria are impacted so are our digestive capabilities. This can lead to maldigestion or imbalances in the fermentation of certain carbohydrates. This can then lead to excess gas being produced, the most common cause of bloating and distention. [7]
Stress and Pain
Stress, as well as poor sleep which often results from stressful life events, contributes to visceral hypersensitivity. This is a heightened response to pain by the nerves within the gut, ie, they become overly sensitive. This means that stress can increase the sensation of bloating without there being more gas produced within the gut.
For many with digestive symptoms, this may be where there is the sensation of increased pressure or irritation in the bowel, but their stomach remains flat and doesn’t expand.
Not only can this lead to irritation in the bowel, but an increased or altered perception of that pain in parts of the brain. [8]
What does anxiety stomach pain feel like?
Anxiety can be felt in the stomach in a number of ways. For many, it can feel very different to the typical feeling of IBS (irritable bowel syndrome) but for others, it can be very similar.
It can commonly be described as:
- Feeling of butterflies in the stomach
- Cramping in the abdomen
- Nausea or feeling the need to be sick
- Alteration in bowel patterns.
For some with digestive issues like IBS, stress and anxiety can increase all of their symptoms. These can often be described as a flare-up. [9]
Symptoms of Stress-Induced Bloating
Stress can impact many aspects of health. Where it impacts an individual may be due to an increased susceptibility due to genetics. The areas that stress can impact include physical health as well as emotional health but gut also the gut. Not only can digestive symptoms such as bloating be uncomfortable but it can also impact daily life.
Some of the symptoms of stress-induced digestive symptoms may be obvious, but there are also less common symptoms that appear. Understanding the causes of these symptoms can help to identify the underlying reasons. This can not only help with managing symptoms but also treatment options.
Physical Symptoms:
- Excessive Gas: Alterations in the gut microbiome may lead to higher levels of gas being produced in the bowel.
- Feeling of Fullness: Gas and increased sensitivity along the gut lining can lead to feeling overly full, even when eating little.
- Abdominal Pain: Nerve sensitivity as well as cramping can be 2 main factors responsible to increased pain.
Digestive Changes:
- Altered Bowel Habits: Changes in stress and gut microbiome imbalances may contribute to constipation or diarrhoea.
- Heartburn: Combinations of gas production, acid and nerve sensitivity can contribute to symptoms at the upper end of the digestive tract.
- Increased Bowel Sounds: Bowel function changes can lead to noises, described as borborygmi.
Emotional and Psychological Symptoms:
- Increased Anxiety: While anxiety can impact the gut, alterations in the gut can contribute to stress, creating a vicious cycle.
- Mood Swings: During flare-ups of symptoms more stress can appear, leading to changes in mood.
- Loss of Appetite or Stress Eating: Sensations of nausea and feeling overly full can contribute to a loss of appetite. In some patients, appetite and comfort eating may increase during stressful times.
Impact on Daily Activities:
- Discomfort During Activities: Abdominal discomfort, pain and unpredictable bowel patterns can impact daily life, restricting activities.
- Sleep Disturbances: Pain, bloating and stress all contribute to poor sleep. In turn, poor sleep may aggravate these symptoms.
Common Questions About Stress and Digestive Health
How long does stress bloating last?
If bloating happens when stress levels rise, these gut symptoms can calm down fairly soon after the stress is no longer present. However, for some, there may still be a level of sensitivity in the gut.
In these situations, many people, following a stressful event or stressful time in their lives there bloating has carried on. This may be due to changes area such as the gut-brain connection or the gut microbiome, leading to alterations in gut function and ongoing symptoms. [10]
Can stress cause other gastrointestinal problems?
Bloating rarely comes in isolation and can often be attributed to imbalances in the microflora, which can be caused or worsened by daily life stress. During prolonged periods of stress gut microbiome diversity is impacted.
Gut microbiome diversity is a key indicator of the health of the microbiome. Once the diversity of key bacteria is lost then the function of the entire ecosystem is impacted.
This may then lead to:
- Increased risk of digestive issues such as IBS
- Increased risk of inflammatory bowel conditions such as Crohn’s and Ulcerative Colitis
- Disruption of the gut-brain axis and the stress response. For example, increasing how sensitive we are to stress.
- Increased risk of metabolic conditions such as type 2 diabetes and obesity. [11]
When should I seek medical advice?
Medical advice can be considered for any ongoing digestive issues. However, certain symptoms are considered ‘red flag’ symptoms. This means that medical advice should be sought to rule out any underlying factors apart from stress.
These red flag symptoms include:
- Abdominal or rectal masses
- Rectal bleeding
- Unexplained weight loss
- A family history of bowel or rectal cancer
- A family history of ovarian cancer
- Those over 60 years of age experiencing a change in bowel patterns lasting longer that 6 weeks [21]
Practical Steps to Manage Stress-Induced Bloating
When bloating is present, there are several strategies that can be used to calm both the stress and the gut. A lot of the time, the combination of several of these may be more beneficial than a single one.
Breathing Practices
Diaphragmatic breathing is a key component for calming the central nervous system. This is also known as belly breathing and involves activating the diaphragm by breathing from the belly.
When in times of stress or anxiety we can see that our breathing changes from deep belly breaths to breaths that are shallower and originate from the chest. These shallower breaths can almost be seen as a mild form of hyperventilation, further activating the fight or flight response and contributing to bloating. [12]
Gut Directed Hypnotherapy
A well-researched approach to calm and support the gut-brain connection is gut-directed hypnotherapy. This can be used to calm the gut-brain connection and the vagus nerve. It also introduces practices to calm abdominal cramping and muscle relaxation.
Since stress and anxiety may contribute to muscle tightening, these can be used to support the physical as well as the emotional. [13]
Probiotics
Probiotics are supplements (capsules or powders) containing beneficial bacteria. Several strains have been found to improve a wide range of digestive symptoms including IBS and bloating.
Further supplements have been found to improve mood and reduce stress via the gut-brain connection. Rather than these being termed probiotics, the term psychobiotic is used. [14]
Prebiotics
Prebiotics are soluble fibre powders that support the beneficial bacteria in the gut. These can be considered as the fertiliser for the bacteria we already have.
Many people with IBS or bloating find that prebiotics introduce too much fibre and may increase symptoms. However, research indicated that prebiotics can improve the microbiome and the gut-brain connection
For example, galactooligosaccharide (in the product BIMUNO) can improve digestive symptoms. However, starting with a low amount is often needed. This same prebiotic has also be found to improve depression and anxiety.
Herbal Supplements
Key calming herbs can be particularly helpful under periods of acute stress and are commonly available in tea or supplement form:
- Valerian
- Skullcap
- Lemon Balm [15]
Additionally, adaptogenic herbs that help the body to adapt to stress may take a little longer to build up within the body but can offer significant benefits:
- Ashwagandha
- Rhodiola
- Siberian Ginseng [16]
Digestive Enzymes
Enzymes are produced in the digestive system by the pancreas, the liver as well as the cells along the lining of the small intestine.
Due to irritation or microbial imbalances in the gut, food may not be properly digested leading to symptoms. Digestive enzymes can be taken as a supplement to aid in the digestive processes. [17]
Simethicone
Simethicone is the ingredient in products such as Wind-eze and helps to relieve gas, bloating and trapped wind. This works by breaking smaller gas bubbles down to create a big bubble of gas which is easier to pass. [18]
Activated Charcoal
Charcoal is used to help relieve bloating by absorbing gas in the gut. It would need to be taken at least 2 hours away from any medication. Additionally, those with constipation may need to avoid this supplement as it can slow the bowel further. [19]
Dietary Considerations to Reduce Bloating
If someone is experiencing bloating very frequently, it may be best to avoid specific fibres which commonly contribute to increased gas production. These are commonly referred to as FODMAPs and include:
- Garlic
- Onion
- Wheat
- Beans
- Lentils
Related article: Low FODMAP Foods: Everything You Need To Know
Even if certain foods are restricted, it’s important to keep the diet as diverse as possible. Dietary aims to keep in mind are:
- Aiming for at least 30 different plant foods a week. These plant foods include fruits, vegetables, herbs, spices, and herbal teas.
- Aiming to eat each colour of the rainbow every day. This strategy helps to ensure a diet that supports a diverse gut microbiome.
- Including fermented foods in the diet. These include kimchi and sauerkraut.
Stress and Bloating: The takeaway message
Stress is one of the most common factors in modern life and leads to a wide range of health issues.
Understanding our individual stress triggers and when and where we’re exposed to them is a key component to support both our emotional health and our digestive health.
It is often the case that both areas need support. Our emotional health with a caring and nurturing approach to ourselves through stress management and self-awareness practices.
Our digestive health through a diverse and colourful diet, the use of specific supplements, and potentially restricting specific foods that may increase bloating and gas.
If you’re experiencing bloating and need support, contact us for a free assessment.
References
- Max Schmulson, MD. Understanding Bloating and Distension
- Ahmad, Asma Hayati, and Rahimah Zakaria. (2015). Pain in Times of Stress.
- Thau L, Gandhi J, Sharma S. (2023) Physiology, Cortisol.
- Khoshbin K, Camilleri M. (2020. Effects of dietary components on intestinal permeability in health and disease.
- Ohlsson L et al (2019. Leaky gut biomarkers in depression and suicidal behavior.
- Foster, Jane A et al. (2017). Stress & the gut-brain axis: Regulation by the microbiome.
- Seo, Ye Seul et al. (2020). Dietary Carbohydrate Constituents Related to Gut Dysbiosis and Health.
- Rengarajan S et al (2020). A Potential Role for Stress-Induced Microbial Alterations in IgA-Associated Irritable Bowel Syndrome with Diarrhea.
- Ceuleers, Hannah et al. (2016). Visceral hypersensitivity in inflammatory bowel diseases and irritable bowel syndrome: The role of proteases.
- Patel, A et al. (2016) Effects of disturbed sleep on gastrointestinal and somatic pain symptoms in irritable bowel syndrome.
- Greenwood-Van Meerveld, Beverley, and Anthony C Johnson. (2017). Stress-Induced Chronic Visceral Pain of Gastrointestinal Origin.
- Wei, Lai et al. (2021). Gut microbiota dysbiosis in functional gastrointestinal disorders: Underpinning the symptoms and pathophysiology.
- Liu, Jie et al. (2022). Slow, deep breathing intervention improved symptoms and altered rectal sensitivity in patients with constipation-predominant irritable bowel syndrome.
- Bannach-Brown, Alexandra et al. (2019). Administration of galacto-oligosaccharide prebiotics in the Flinders Sensitive Line animal model of depression.
- Tammadon, Mohammad Reza et al (2021). The Effects of Valerian on Sleep Quality, Depression, and State Anxiety in Hemodialysis Patients: A Randomized, Double-blind, Crossover Clinical Trial.
- Panossian, Alexander, and Georg Wikman. (2010). Effects of Adaptogens on the Central Nervous System and the Molecular Mechanisms Associated with Their Stress-Protective Activity.
- Spagnuolo R, et al. (2017). Beta-glucan, inositol and digestive enzymes improve quality of life of patients with inflammatory bowel disease and irritable bowel syndrome.