Inflammatory bowel diseases impact over 7 million people in the world. Over recent years there have been significant advances in treatments However, some patients will still require a surgery that results in a stoma.
This guide offers compassionate, evidence-based support for patients, families, and carers.
Key Stats
- 46% prevalence of depression post-stoma surgery
- 85% had peristomal skin complications; 43% experienced leakage onto clothing
- Only 16.6% of diverting stomas for perianal Crohn’s achieve successful reconnection
- 82% of patients couldn’t recall receiving exercise advice during recovery
- 50% of sexually active patients do not resume activity post-surgery
- Only 6% of UK IBD services meet psychological support staffing recommendations
- 20–40% of ileostomy patients experience dehydration post-operatively
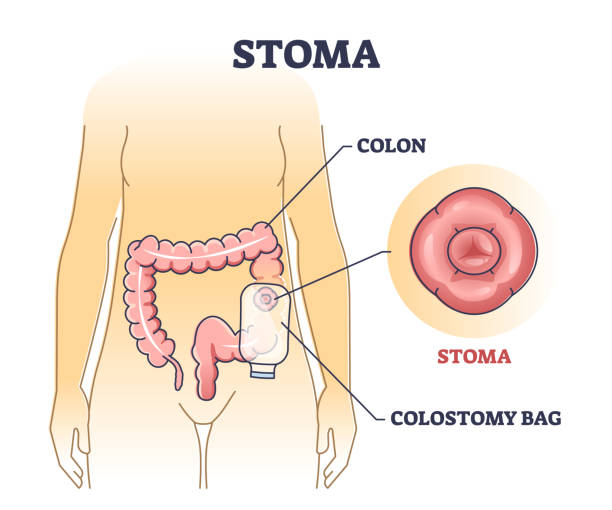
What is a Stoma?
When part of the bowel is impacted or removed, a stoma is where the bowel is divered to an opening in the belly. This then allows for the stool (poo) to be collected in a bag on the surface.
Stats
- In the UK, around 2,000 IBD patients undergo stoma surgery annually
- In the US, up to 1 million people live with an ostomy
The most common forms of stomas are Ileostomies which involved the small bowel.
Stoma-related issues can happen in a high number of patients. Some studies indicated this to be up to 70% of patients, making understand of stoma issues and specialist support essential.
Types of Stomas for IBD Patients
Ileostomies are the most common in IBD and are names as such due to this involving the ileum, the second of the small bowel. This is different to colostomies which involce the colon.
Loop stomas are more common in the small bowel also, these commonly only short-term following some form of IBD related bowel surgery. These are different to end stomas which are considered a permanent diversion of the bowel.
Stats
- Only 16.6% of patients with diverting stomas for Crohn’s achieve successful bowel reconnection.
- Complications are significantly higher in Crohn’s (36.8%) than ulcerative colitis (17.4%).
The Stoma Surgery Process
The stoma process involves 3 main steps.
- Step 1 – Pre-operative Preparation. This involves the decision around what type of stoma is needed. This also involves the decision of the exact location to avoid skin folds, any scars and the waistline. This to reduce complications and leakage of the stoma bag, once fitted.
- Step 2 – The Surgery. Once the damage part of the bowel has been removed, the bowel is then attached to the opening that has been created in the abdominal wall. This is stitched into place and a stoma bag fitted.
- Step 3 – Post-Operative Recovery. This is where the stoma bag starts to fill and healing of the surgery begins. The patient is also given guidance and taught how to case for the stoma to prevent complications.
- Regular stoma nurse follow-ups in the first year are essential for managing pouch fit, skin health, output, and emotional wellbeing.
Emotional and Psychological Impact
It’s well understood that emotional impact of having a stoma. This can include both depression and anxiety that are both present in around 50% of those with a stoma.
A 2023 Psychiatry meta-analysis found:
- 46% prevalence of depressive symptoms after stoma surgery.
- 47.6% prevalence of anxiety after stoma surgery.
Additional studies have also found that only 6% of UK IBD services meet psychological support staffing recommendations.
Further emphasising the importances to emotional support and ensuring it’s in place, 77% of ostomy patients with depression/anxiety report never receiving formal support.
Caring for Your Stoma & Managing Leaks
Emotional wellbeing is closely link to leaks and the fear of leaks. Therefore, ensuring stomas are well looked after is important for practical and emotional reasons.
There is also a clear link between leakage onto clothing, how this leads to skin complications and then lower emotional wellbeing.
Practical tips:
- ensure correct pouch sizing
- use barrier rings for uneven skin
- change pouches proactively
- elastic tapeless barriers reduced leakage risk by 41%
Diet and Nutrition Considerations
Dietary approaches can be highly individual. However, as a guide a lower fibre can be helpful for the first 2 months to support healing. Longer that this can contribute to malnutrition which is reported to impact 40-79% of ileostomy patients.
Following this, a higher fibre, Mediterranean style diet is to be considered. This has been shown to help improve weight, reduce dehydration and lower rates of hospitalisation.
Physical Activity and Exercise
Hernias can affect up to half of stoma patients but physical activity has been shown to improve outcomes and reduce the need to repair surgry.
It is also not uncommon for patients to not recall being having given advise on this aspect of repair and long-term outcomes.
The HALT trial showed Pilates-based exercises improved hernia size, abdominal control, and body confidence.
Sexual Health and Intimacy
Stoma can impact body image and increase concern about leakage from the bowels. Up to 50% of those with a stoma do no resume sexual intimacy following surgery which makes it important for there to be an open and supportive conversation around the gut and stomas.
Key Tips
- Empty the pouch before intimacy
- Use opaque or mini pouches
- Wear wraps to conceal
Travel Tips
Being out of the normal routine can impact bowel function. This is amplified with air travel, often due to the change in cabin pressure.
- Pack extra supplies and include them in carry-on and in hold luggage
- Request a travel certificate from the IBD team or stoma nurse
- As stoma pouches may expand at altitude with the cabin pressure drainable bags for flights can help reduce any possible accidents
- Stoma charities (Colostomy UK, UOAA) provide multilingual travel cards explaining your condition and need for supplies and accessible toilets in the can or urgent need.
Common Myths
Several myths can persist around stomas and their long-term impact.
Here are the most common myths busted.
| Myth | Reality |
| “You can’t exercise” | Exercise reduces hernia risk and improves quality of life |
| “Everyone will notice” | Modern pouches are discreet and odour-proof |
| “Your sex life is over” | Most who resume activity report satisfaction. |
| “A stoma means things have gone wrong” | For many, it’s a planned, positive step toward freedom from uncontrolled disease.
|
Conclusion
A stoma is unboundedly a major life adjustment. However, with the right proactive care and support it should not be seen as a barrier to living a full life.
Contact us today at The IBS Gut Health Clinic and find out more about how we can support you throughout this journey.
Last Updated
Published by Martin Cohen on 15/03/2026
References
- MDPI (Healthcare) — The Prevalence of Leakage, Peristomal Skin Complications and Impact on Quality of Life in the First Year Following Stoma Surgery
- PubMed (Alimentary Pharmacology & Therapeutics) — Systematic review with meta-analysis: faecal diversion for management of perianal Crohn’s disease
- Pilot and Feasibility Studies (BMC) — Hernia Active Living Trial (HALT): a feasibility study of a physical activity intervention for people with a bowel stoma who have a parastomal hernia/bulge
- Journal of Wound Ostomy & Continence Nursing — Pouching System Leakage and Peristomal Skin Complications in New Stoma Patients
- IBD UK (British Society of Gastroenterology) — IBD UK Report: The State of IBD Care in the UK
- PMC (Gastroenterology & Hepatology) — Psychological Considerations and Interventions in Inflammatory Bowel Disease Patient Care
- British Journal of Nursing — Hernia Active Living Trial (HALT): an exercise intervention in people with a parastomal hernia or bulge
- PMC (Colorectal Disease) — Probability of Stoma in Incident Patients With Crohn’s Disease in Sweden 2003–2019: A Population-based Study
- Crohn’s & Colitis Foundation — IBD and Mental Health: Healing Beyond the Gut